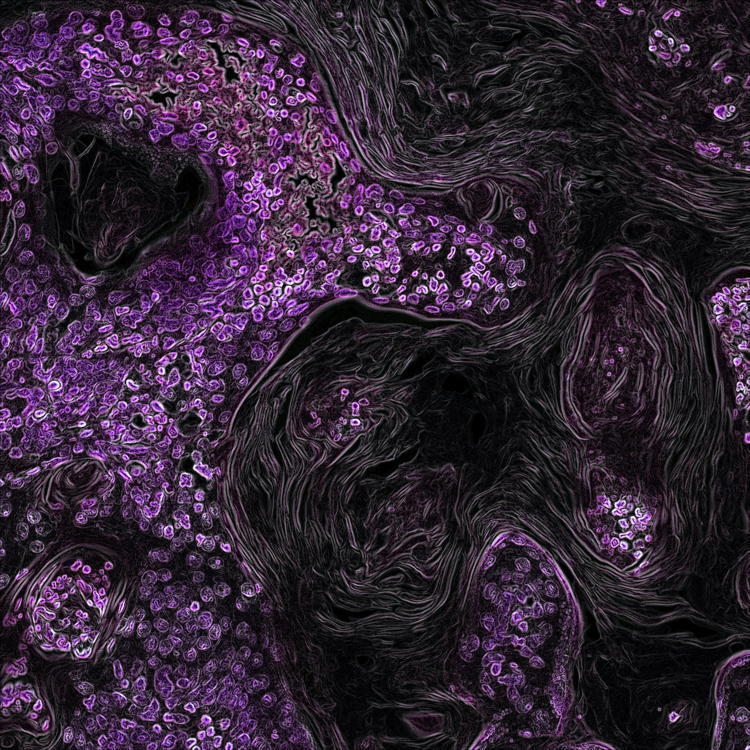
Changes in cytoplasmic and extracellular neuromelanin in human substantia nigra with normal aging
Submitted: 31 May 2021
Accepted: 22 July 2021
Published: 1 September 2021
Accepted: 22 July 2021
Abstract Views: 1045
PDF: 498
HTML: 12
HTML: 12
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Similar Articles
- Zhijiang Chen, Huili Wang, Bin Hu, Xinxin Chen, Meiyu Zheng, Lili Liang, Juanjuan Lyu, Qiyi Zeng, Transcription factor nuclear factor erythroid 2 p45-related factor 2 (NRF2) ameliorates sepsis-associated acute kidney injury by maintaining mitochondrial homeostasis and improving the mitochondrial function , European Journal of Histochemistry: Vol. 66 No. 3 (2022)
- A. Bolekova, T. Spakovska, D. Kluchova, S. Toth, J. Vesela, NADPH-diaphorase expression in the rat jejunum after intestinal ischemia/reperfusion , European Journal of Histochemistry: Vol. 55 No. 3 (2011)
- F. Dorko, T. Å pakovská, K. Lovasová, P. PatleviÄ, D. Kluchová, NADPH-d activity in rat thymus after the application of retinoid acid , European Journal of Histochemistry: Vol. 56 No. 1 (2012)
- Minkai Cao, Deping Yuan, Hongxiu Jiang, Guanlun Zhou, Chao Chen, Guorong Han, Long non-coding RNA WAC antisense RNA 1 mediates hepatitis B virus replication in vitro by reinforcing miR-192-5p/ATG7-induced autophagy , European Journal of Histochemistry: Vol. 66 No. 3 (2022)
- Bo Dai, Hailin Liu, Dingmin Juan, Kaize Wu, Ruhao Cao, The role of miRNA-29b1 on the hypoxia-induced apoptosis in mammalian cardiomyocytes , European Journal of Histochemistry: Vol. 68 No. 3 (2024)
- Manuela Malatesta, Histochemistry for nanomedicine: Novelty in tradition , European Journal of Histochemistry: Vol. 65 No. 4 (2021)
- V. Insolia, V.M. Piccolini, Brain morphological defects in prolidase deficient mice: first report , European Journal of Histochemistry: Vol. 58 No. 3 (2014)
- Manuela Monti, CarloAlberto Redi, Ernesto Capanna, Genome size evaluations in cockroaches: new entries , European Journal of Histochemistry: Vol. 66 No. 2 (2022)
- Chaojie He, Yi Yu, Feifan Wang, Wudi Li, Hui Ni, Meixiang Xiang, Pretreatment with interleukin-15 attenuates inflammation and apoptosis by inhibiting NF-κB signaling in sepsis-induced myocardial dysfunction , European Journal of Histochemistry: Vol. 68 No. 2 (2024)
- Qingjing Gao, Wenqian Xie, Wenjing Lu, Yuning Liu, Haolin Zhang, Yingying Han, Qiang Weng, Seasonal patterns of prolactin, prolactin receptor, and STAT5 expression in the ovaries of wild ground squirrels (Citellus dauricus Brandt) , European Journal of Histochemistry: Vol. 67 No. 4 (2023)
<< < 31 32 33 34 35 36 37 38 39 40 > >>
You may also start an advanced similarity search for this article.

 https://doi.org/10.4081/ejh.2021.3283
https://doi.org/10.4081/ejh.2021.3283